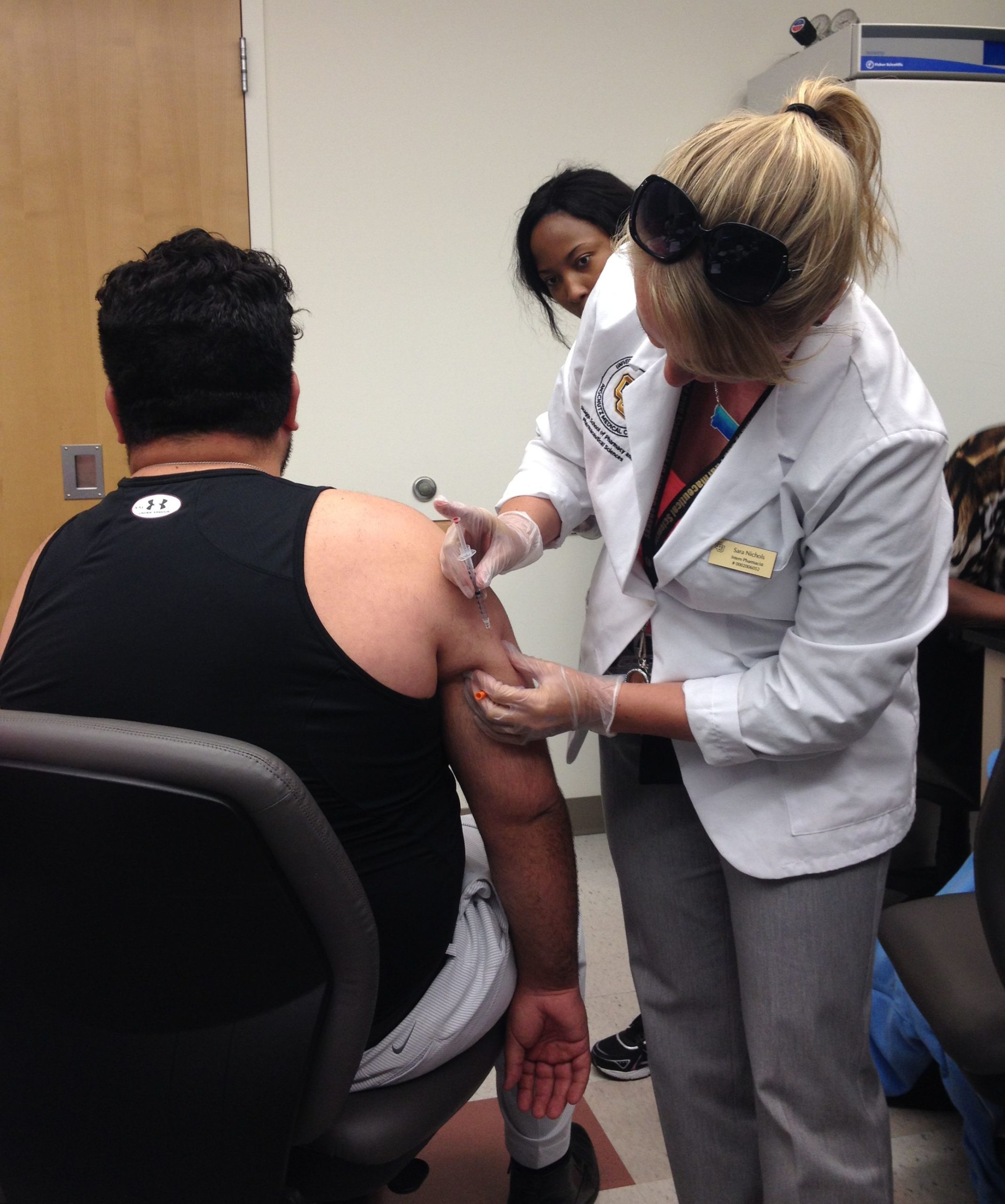
My colleagues and I from the University of Colorado School of Pharmacy were “on the air” last week at 9News in Denver answering vaccine questions at 6:45am. We were surprised that so many of the calls we received expressed concerns about vaccines, until we noticed the ticker across the bottom of the screen streaming “if you have concerns about vaccines, call …”.
I spoke with one dad who was concerned about his 11 year old son receiving the Human Papilloma Virus, or HPV, vaccine. “Does my son really need this?” I explained that the HPV vaccine provides protection from genital warts and cervical cancer. “So, does my 11 year old really need this?”
Good question. If only we knew how our lives would unfold, we could make the very best vaccine decisions. If the boy is going directly on to become a celibate monk, the HPV vaccine will provide protection the son probably won’t need. If only the dad could rely on the boy to discuss sexual activity seven months in advance, the HPV vaccine could be delayed until it’s actually “needed”. If only the son knew the sexual history of all his future partners, he might not even need the vaccine.
But, HPV is the most common sexual transmitted infection in the US.
While most infections produce no clinical symptoms and no disease, HPV can result in genital warts and cancers in both men and women. HPV is thought to be responsible for nearly all cases of cervical cancer. There is no specific treatment for HPV infection, although genital warts, abnormal cervical changes and cancers can be treated, so, we have the HPV vaccination.
- The vaccine is a three shot series.
- The second dose is administered 1-2 months after the first shot;
- the third and last shot is given six months after the first one.
- The vaccine is recommended prior to HPV exposure through sexual contact, and is recommended for those as young as 13 years old up to age 26.
The most common adverse reactions following HPV vaccination are pain, redness or swelling at the injection site; these occur in up to 90% of patients and can worsen with subsequent shots in the series. According to the CDC Pink Book, NO serious adverse events to the HPV vaccination have been reported to the FDA or CDC. More than 99% of vaccinated individuals will be immune to HPV after completing the three month series.
As we are making vaccine decisions, we don’t know if our children will be exposed to diseases like diphtheria, tetanus, whooping cough, measles, mumps, rubella, chicken pox, or sexually transmitted diseases such as human papilloma virus.
The vaccine is always a better choice than catching the disease.
One of our 9News callers was pretty upset about vaccinations and suggested we needed to look into the harm caused by vaccines. Good point. Any problem developing after vaccination might be assumed to be due to the vaccination. The FDA has a Vaccine Adverse Effect Reporting System which requires health care professionals to report all suspected vaccine-related adverse effects. Monitoring these reports allows identification of adverse effects that occur more frequently following vaccination than otherwise. This is the scientific way to identify the true adverse effects to vaccines.If something happens following a vaccination, you tell all your friends and may even put it on the internet.
Meanwhile, the benefits of vaccination are statistical events that do not occur, diseases that you don’t get because you’ve been vaccinated.
I know of no internet reports of children who did NOT catch measles because of the vaccine, even though 90% of children used to get measles and now almost no one gets measles. No internet reports of the 1 in 500 children who did NOT die from measles. No internet reports of the 1 in 100 children who do NOT have seizures following measles. No internet reports from people who might otherwise have genital warts, but don’t.
It’s important to compare benefits and risks for all treatments, including medicines and vaccines. The CDC’s Advisory Committee on Immunization Practices examines benefits and risks to makes vaccine recommendation for children and adults. Some vaccines have a favorable balance of benefit to risk and some don’t unless special circumstances apply. You’re unlikely to have the rabies vaccine unless you’ve been exposed to rabies. Some vaccines (like cholera vaccine) are available, but NOT recommended unless you’re traveling to certain places.
August has focused on National Immunization Awareness and September marks the start of flu vaccine season. If you have questions or aren’t sure of what vaccinations are recommended, it’s OK to talk to you doctor, nurse or pharmacist.