Background
Opioids are a type of medication that works to reduce the intensity of pain and work very well for this purpose. However, opioids also have the potential for overuse, abuse, and/or addiction. Heroin is also an opioid drug in the illicit form. These drugs all have potential for overdose and death if taken inappropriately. For example, people who take opioid pain medications with a valid prescription may misunderstand the directions, accidentally take too much, or purposely misuse the medication. Sometimes overdoses can happen if opioid medications are mixed with other depressing substances, including other medications, alcohol, or over the counter medications. Overdoses are common in illicit drug use as well because it is hard for people to know exactly how much of a drug they are truly ingesting if it is bought off the street. Fortunately, there is an opioid reversal agent available called naloxone.
What is naloxone?
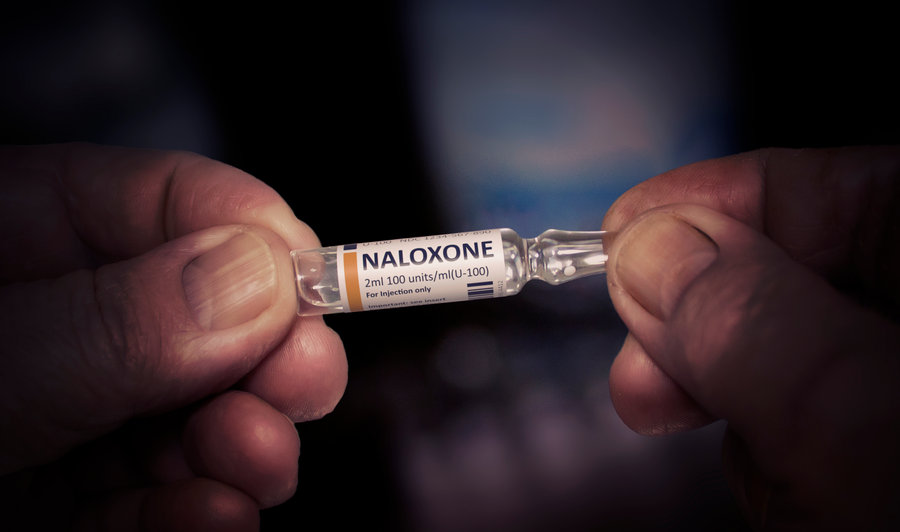
Naloxone is a medication used to reverse and block the effects of opioids like heroin, morphine, and oxycodone. It works by binding to the opioid receptors, where the opioid drug normally would bind to take effect, and blocks the opioid drug from working. When used in the case of an overdose, naloxone rapidly reverses the opioid overdose. However, naloxone treatment is only temporary and sometimes requires multiple doses to continue working or to even start working in cases of severe overdoses. Naloxone is either given as a nasal spray, shot into the muscle, shot under the skin, or intravenous injection. Until recently, naloxone had only been approved by the FDA (Food and Drug Administration) in a dose of 2mg or 4mg for nasal spray products. In April 2021, though, the FDA approved a higher dose of the medication at 8mg to be used as a nasal spray in the treatment of opioid overdose. This will help in those cases where someone needs a higher dose to reverse the effects of the opioids they’ve ingested.
Who should have access to naloxone?
According to the Substance Abuse and Mental Health Services Administration (SAMHSA – see resource 4), candidates for naloxone are those who:
- Take high doses of opioids for long-term management of chronic pain
- Receive rotating opioid medication regimens
- Have been discharged from emergency medical care following opioid poisoning or intoxication
- Take certain extended-release or long-acting opioid medication
- Those who have had a period of abstinence to include those recently released from incarceration.
Be sure to understand the signs and symptoms of opioid overdose if you are a naloxone candidate or know someone who uses opioid medications. Signs of overdose might include finding someone unresponsive and not responding to touch or voice, slowed or not breathing, pin-point sized pupils, and/or bluish lips and nose.
How can you get naloxone?
You can purchase naloxone from a pharmacy without a prescription in many states. You can also get a prescription from a doctor to take to the pharmacy and see if your insurance will cover the medication. Many states have programs available to get naloxone free to those in need as well. If you are not sure what to do to get naloxone, ask your healthcare provider or pharmacist.
Resources:
- https://www.fda.gov/news-events/press-announcements/fda-approves-higher-dosage-naloxone-nasal-spray-treat-opioid-overdose
- https://www.cdc.gov/opioids/data/index.html
- https://www.mayoclinic.org/diseases-conditions/prescription-drug-abuse/in-depth/how-opioid-addiction-occurs/art-20360372
- https://www.samhsa.gov/medication-assisted-treatment/medications-counseling-related-conditions/naloxone