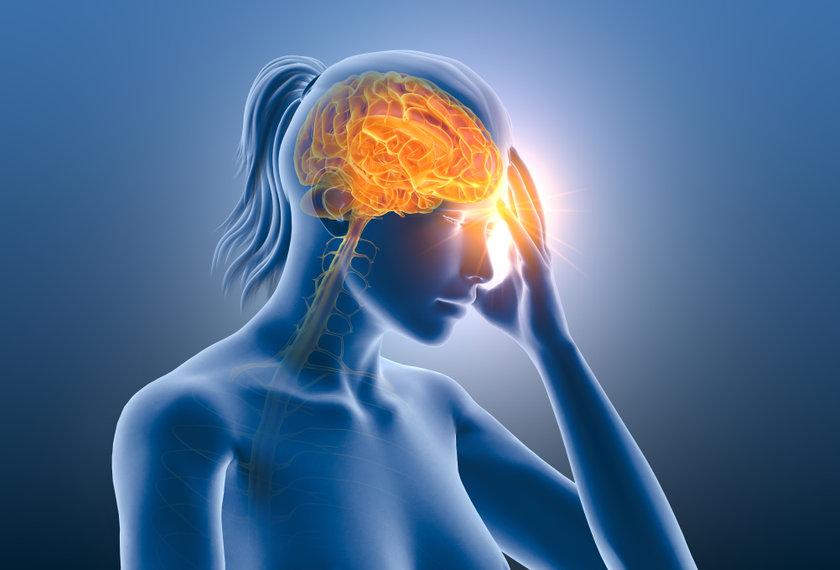
Headaches are one of the most common and nonspecific conditions experienced by people of all ages and all backgrounds. To be alive is to experience a headache from time to time. By properly managing our diet, stress, and lifestyle, we can do our best to prevent them; however, despite our best efforts, some are inevitable. Headaches range from very mild to very severe, each with their own causes for concern and associated symptoms. Among the headache population, those who experience migraines are most affected. Migraines are a type of severe headache that are often accompanied by other symptoms including nausea, fatigue, light sensitivity, and even changes in vision.
A migraine in its simplest form is caused by changes in electrical signals and blood flow. These changes can occur nearly anywhere in the brain, but interesting symptoms arise when they happen in the part of the brain that processes vision, the occipital lobe. Our eyes are highly complex structures, but they are nothing compared to what’s going on behind them. The path from the eyes to the brain is unimaginably complex, and it is primarily responsible for vision as we know it.
When a person has a migraine that includes the area for visual processing, we “see” our migraine rather than feel it. This condition is called an ocular migraine. Ocular migraines can occur alone or be associated with a headache. Often patients will experience an ocular migraine prior to their “actual” migraine. This is referred to as a prodrome, a type of warning sign that a migraine is on its way. Ocular migraines are characterized by a blind spot in the vision that usually starts small, grows to about a third of the visual field, lasts around 30 minutes, and resolves spontaneously. These blind spots can vary widely depending on the patient. A classic description is an arc shaped, twinkling image to the left or right hand side. Although the name “ocular migraine” may sound as though something is going on in the eye, this is a neurological phenomenon. There is no long-term risk for eye damage or vision loss associated with ocular migraines. When these occur, I advise patients to simply relax in a safe and quiet space until the symptoms resolve.
Read more about Novel Treatments for Migrains
Prevention and treatment strategies for ocular migraines are similar to standard migraines, including lifestyle modifications and avoiding triggers. In my experience, patients will have one or two episodes a year, though some may have more or less. I first advise patients to follow up with their primary care physician to ensure their overall health is stable. Sometimes a consult with a neurologist is recommended if the episodes are frequent or severe. It is also helpful to keep a “headache journal”. Documenting the time and surrounding events of a migraine can help patients avoid future attacks.
This being said, there are several other eye and neurological conditions that can cause symptoms mimicking an ocular migraine. If you’re experiencing flashes of lights or blind spots in your vision, I strongly recommend seeing an eye doctor as soon as possible to rule out other potential causes. For more information, talk to your doctor, and see the links below.
References:
https://www.aoa.org/healthy-eyes/eye-and-vision-conditions/ocular-migraine?sso=y
Understanding Ocular Migraine